- Health Blog
- Health Blog
Dermatitis
Written by: Editors
Modified on:

It is usually a surprise to learn the skin is the largest organ of the human body. However, it is then less surprising to learn that skin conditions like dermatitis are very common. As it is such a frequent irritant, let us scratch beneath its surface…
What is it?
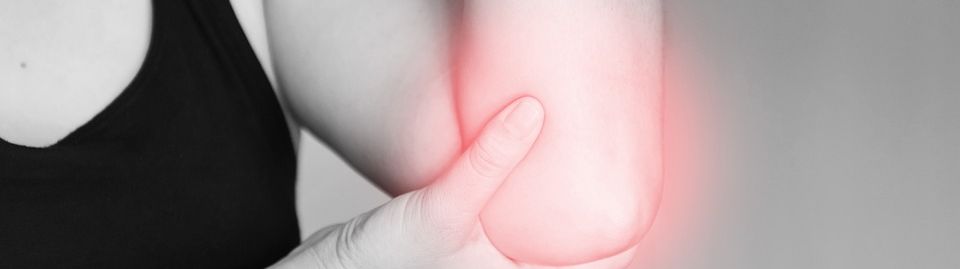
Dermatitis refers to inflammation of the skin with characteristic features of itchiness, red skin and swelling. Any size area of skin can be involved and it can occur anywhere – from a localised area to large separated areas. Common areas affected are the hands, arms, neck and genitals.
How many types are there?
There are many causes and so many types of dermatitis. However, three predominate atopic, irritant contact and allergic contact dermatitis.
1 Atopic
Atopic dermatitis is what is usually called ‘eczema’ (although this term is used interchangeably with many forms of dermatitis) where flares and remissions of widespread itchy red and scaly skin occur – particularly in the skin folds of the arms, knees, wrists and hands. It is an internal response involving the immune system.
Atopic dermatitis is caused by a combination of genetic predisposition and environmental trigger (like asthma). Typical triggers include atmospheric conditions, skin products and stress.
2 Irritant contact
Irritant contact dermatitis, however, is caused by an outside stimulus triggering a local outside on the skin. It occurs within 12 hours of exposure and usually only in areas in direct contact where the irritant chemicals penetrated the skin barrier. It does not involve the systemic immune system. Typical irritants are soaps, detergents and solvents like perfume components.
3 Allergic contact
Meanwhile, allergic contact dermatitis is caused by an outside stimulus that triggers the systemic immune system slowly, taking up to 48 hours to manifest. It usually shows on the second time of contact (the first merely sensitizes the skin) e.g. a red circle beneath a nickel button on jeans on the second time of wearing. It accounts for only 20-25% of contact cases.
4 Other Types
There are many other types o including; seborrheic dermatitis (flaking scalp and face triggered by a skin living fungus), xerotic dermatitis (reacting to dry conditions typically in winter), stasis eczema (caused by venous blood collecting in ankles irritating the skin), neurodermatitis (secondary to repeated scratching
irritating the skin) and herpetiformis (small collection of bumps on the back/elbows/knees associated with intestinal disease.)
How is it diagnosed?
In most, a detailed history of potential triggers and detailed examination of affected skin leads to the diagnosis. However, where the diagnosis is difficult or doubtful due to persistent or treatment-resistant symptoms, further tests may be helpful.
Patch testing wherein a panel of 25-40 allergens is stuck to the back and reviewed on day 2 and day 4 to assess for presence and speed of reaction differentiates between types of contact dermatitis.
Meanwhile, for atopic eczema, allergy tests include skin prick tests, blood tests (IgE and RAST for immune response) and sometimes a skin biopsy where necessary.
However, the tests are not entirely accurate and interpreting them appropriately requires judgement by a doctor who knows the individual patient situation.
How is it treated?
Treatment for dermatitis follows the same principles despite the different causes.
First are lifestyle interventions – the most vital being removal of potential triggers or irritants from the environment. In cases of irritant contact dermatitis, protective precautions must be taken if being exposed to the irritant.
Second are barrier creams and emollients to coat the skin, protecting it from outside forces while also locking moisture within. They are applied liberally and frequently, either directly or as part of a bandage wrap.
Third are stronger medications that work against inflammation, such as steroids and immunosuppressants. Steroids reduce immune system activity and are typically used as creams alongside the barrier creams. They can also be taken by mouth for a whole body response if needed.
Less frequently, immunosuppressive creams or tablets are added for more direct action to prevent the body from mounting the response that leads to the symptoms in the first place.